 I took Anatomy in high school, but I guess I wasn't paying much attention when we learned about the heart. No matter how many doctors I talk to, I can't seem to get a good grasp on my baby's heart defect and pulmonary hypertension. Yesterday my mother-in-law sent a letter to my older son explaining why his brother needs the constant low-flow oxygen he has recently been prescribed. It is the best description I've ever read: Hi again Caspian! I wanted to tell you a story about why your brother needs oxygen, and what the doctors will be fixing in his heart when he gets a little bigger.... Think of Benny's heart and lungs as a little house, with a furnace to keep it warm. It's cold outside, and Benny's little house has a door, and a window, and that furnace. Because it's cold outside, Benny likes, and needs, to have a warm little house. Benny has to go outside frequently to get supplies--food, air, and wood for his furnace. Every time he goes outside, he opens the door and then closes it behind him, so the house won't get cold. But Benny's door doesn't close quite right. The door to YOUR house opens only one way on its hinge, and it closes tight when it closes. Then to open it, it takes some effort.... you have to turn the knob, and pull it open. And when the wind is blowing hard outside against it, even in a storm, the door doesn't blow open on its own. It's SHUT, and shut tight. But Benny's door to his house is more of a swinging door. It sometimes moves BOTH ways, and if there's a big wind outside, the pressure can blow it open and let the cold air in, even though Benny wants his house to stay tight and cozy warm. Sometimes that door is just not tight. Also, Benny's window doesn't quite close. The glass doesn't go all the way down to the bottom--there's a few inches that are always open. The window wasn't measured absolutely correctly when it was made. So cold air is always coming into Benny's little house. That makes the furnace work overtime, and harder than it should. In the real world, Benny now has oxygen--which you can think of acting in Benny's little imaginary heart and lung house as being an extra heater. It takes some of the burden off his furnace in keeping his house warm. It also acts sort of as super fuel for his furnace itself, and protects it from getting overworked. When Benny has his surgery, the doctors will do two things: 1. They will create a bottom to Benny's constantly open window. They'll put another piece of good, strong glass in that window, and then it will shut tight--not letting in any more cold air all the time. When the window has to open, it will open. When it has to shut, it will thus be able to shut. No more always a little open, letting in cold air. 2. They will fix Benny's door. No more swinging open with big winds outside. They will fix it so that it will only open ONE way, and when it closes it will shut tight. When the door has to open to get supplies, it will open, and then shut tight afterwards....not only to not let in cold air constantly, but also to not let those supplies roll away by accident. So then, instead of Benny's little house being cold all the time-- because cold air is always coming in from the window and door that don't shut tight-- thus making his little furnace work so hard, and constantly, to help keep the house warm----with a repaired door and window, his furnace can work normally, like it should, and not so hard all the time. Also, Benny's house will be warmer and more comfortable. Everything will be easier, and more comfortable for Benny, once that door and window are fixed. So until then, the oxygen will help his little furnace--take some of the burden off it by acting as super fuel for it, and also by acting as an extra heater. It isn't heat, though, that's the issue--it's oxygen. Benny's heart and lungs need some help right now to circulate oxygen to his body. Our hearts actually have (what you could call) windows and doors between its chambers (the four "rooms" inside our hearts). They have to open one way, and one way ONLY,and they have to shut tight, and not open up backwards with pressure against them. Those doors and windows are called heart valves. So the doctors will fix up Benny's heart, so that his heart home will stay nice and cozy warm, and his real body will be able to obtain and distribute oxygen well. Then when he gets older, and learns from you and your parents how to run around and ride a bike and swim, his body will have the energy and oxygen to do all that. The doctors know all about how to fix things. Benny just needs to get a little bigger first, before the surgery, and the oxygen he's using now will keep things going okay until that time. You of course can't explain all this to Benny, but when you talk to him,you can tell him that even though sometimes having to have oxygen is blech, it's really helping, and it will be okay. He'll always have someone nearby to take care of him and keep him company. So, big brother--I hope school is fun--your clubs, your friends, your teachers. Send us an Email and tell us when you get a chance. Love, Grandma and Grandpa
5 Comments
If things follow their natural course you get to a point where being pregnant for another second seems worse than whatever it's going to take to get that baby out of your body. At least, this was how it was with my first pregnancy. I gave birth 9 days after my due date. The meat thermometer had long ago popped on that turkey, I was very, very done with being pregnant by the time I finally gave birth. This time things were different. They were different pretty much from the beginning of my pregnancy. After two ectopics and a miscarriage that year, we needed serious reassurance that things were okay. So we started out with an ob at a different hospital in a different city than where we'd gotten the bad news on the previous pregnancies. I just couldn't handle going back to the same ob who kept giving us bad news, even though it had nothing to do with her.  Just when we had started to feel confident that this pregnancy was going to be okay, we got the terrible phone call. Our 20 week ultrasound had revealed a heart defect, and the blood-work had come back 99% positive for Down syndrome. Things were not going at all as planned. Originally we had planned to transfer to a home midwife once we felt confident that things were going well. With the diagnosis that plan went out the window. After the cardiologist okayed us to go back to our original birth plan, but discouraged us from a home birth, I began researching options. I was delighted when the Boulder Nurse Midwives agreed to take us, diagnosis and all. Since they deliver in a hospital this seemed like a great compromise. Then my 1 hour glucose tolerance test came back high. And so did my 2 hour test. Which meant that I had gestational diabetes. I was so angry. I felt like everything that could go wrong in this pregnancy was going wrong.  Checking my blood sugar at home. Checking my blood sugar at home. Despite eating a very restricted diet, which especially sucks when you're pregnant, and taking a walk after nearly every meal, I had several high fasting levels. Since fasting levels are taken first thing in the morning before you eat, there's really no great way to control them with diet and exercise. I eventually figured out through some internet research that eating protein snacks right before bed helps, but the endocrinologist had already recommended insulin. This meant that the Boulder Nurse Midwives couldn't keep me in their practice. I was devastated. Natural birth is important to me. My mom is a nurse-midwife and I grew up with words like "cervix" and "vagina" bandied about the table whenever her midwife friends came over for dinner. My sisters had all had natural births that I had been present for, and I had given birth to my first son naturally. It was a very empowering, wonderful experience that I hoped to have again with my next baby. My biggest fear is having to go into a hospital to give birth and one intervention after another leading to an emergency c-section. It happens all the time. Over 30% of births in the United States are delivered via c-section, a much too high number that reflects the medical mentality that medical intervention now is better than potential litigation later. Being forced to deliver with an OB rather than a midwife put me at much greater risk for interventions, and it was terrifying to me. I deliberated for a week about whether to deliver with a midwife group that could take me with my gestational diabetes, but was all the way down in Denver at the University of Colorado hospital, or if I should go with the obstetrics group and stay at the Foothills hospital in Boulder. Finally I decided to stay in Boulder because I was so uncomfortable in the car already that the prospect of having to drive 45 minutes while in labor didn't seem possible. My sister's good friend Norma had already agreed to come to my birth as a doula, but she had a 6 hour drive to get here, so we also hired a local doula in case she didn't make it. Once I knew I had that support, my stress over the impending hospital birth decreased significantly.  3D ultrasound, creepy or cute? 3D ultrasound, creepy or cute? The gestational diabetes also meant twice weekly non-stress tests, which contrary to the name are very stressful. You're strapped to a monitor for half an hour to determine if your baby is moving often enough. The baby was often sound asleep, and I would spend the half hour eating ice chips to try to wake him up. In addition I had to get an ultrasound every other week to check for hydrops, a type of dangerous fluid retention that can be more common in situations like mine. It was at one of these ultrasounds that the perinatologist told me that she was concerned that I hadn't felt as much movement lately and the baby's growth had slowed down. She thought that it would be safest to induce right at 39 weeks, which happened to be two days later. It was then that I started to cry. I was nowhere near that turning point at which pregnancy is more uncomfortable than the prospect of labor. It seemed like the entire pregnancy was one medical crisis after another, and now it looked like the birth was going to end up the same way. It was too much. Luckily my doula Lisa Waldo was there, and suggested that I let the doctor sweep my membranes to try to get my labor started. This is an uncomfortable procedure where the doctor sticks her finger through your cervix and removes the membranes above it. Not something anyone would look forward to, but if it worked it would be better than getting a Pitocin drip.  I had Max call the troops and let them know labor was imminent. I needed my mother and sisters with me. As much as I hated the idea of induction, having a little bit of a heads up was helpful since they were all coming from far away. For the next few days I tried anything that had been even remotely rumored to help labor get started. Sex, pineapple, spicy food, nipple stimulation, enemas, bouncing on an exercise ball, flower essences, acupuncture...I tried it all. Even if it didn't work, at least some of it was enjoyable. I had been having contractions for days even before the membrane sweep, and they had started to intensify after. The acupuncture I got the next day seemed to kick them into even higher gear. By the time my husband was snoring that night the contractions were ten minutes apart and getting more and more intense. My mom was driving from the four corners area with Norma, my long-distance doula. I was worried that they wouldn't make it in time, and called to tell them my progress so they wouldn't stop for the night. "This is good." my mom said when I told her that I kept seeing bloody show in the toilet and my contractions were getting intense and closer together. I could hear Norma cheering in the background. It takes a special kind of person to cheer over something like bloody show. (Bloody show, also known as the "mucous plug", is just as gross as it sounds. It's the mucous that plugs the cervix up to protect it from bacteria getting in, and it usually comes out right before labor starts.)  The iBirth Contraction Timer The iBirth Contraction Timer Finally my contractions got so intense that my moaning woke my husband up. I had been using the ibirth app to time my contractions, and at that point they were about five minutes apart. He called and was told to bring me in to the hospital. At this point I was very glad that I had opted to stay in Boulder. The one contraction I had during the ten minute car ride was so excruciating that I screamed and swore the entire time while gripping the door handle and attempting to raise my body up off the seat as much as I could. I don't know why, but sitting through a contraction was unbearable for me. I needed to be standing up, moving my hips. This was true throughout my labor. As soon as we arrived I had another contraction in the hospital parking lot. We made our way to the emergency room, which was fortunately empty in the middle of the night on a Thursday. Someone brought a wheelchair over and asked me if I wanted to be wheeled up. "No!" I said emphatically and got a startled look. I couldn't imagine sitting when my contractions were starting to come so close together. We slowly made our way to the elevator, stopping for a contraction along the way. Once we got upstairs the receptionist was expecting us and we were quickly shown to our room. The nurse told us she had read our birth plan, and would do her best to honor our wishes, but she was going to have to set me up on the monitor right now.  Labor monitor print-out. Labor monitor print-out. For the next few hours I was trapped near the monitor because my heart rate was too high. The monitoring reminded me of the non-stress tests, which had not always gone well, and I had been told that if the baby's heart decelerated on the monitor that would cause me to have to have an emergency c-section. This in turn made my heart rate go up, which meant that I had to continue to be monitored, a vicious cycle. If they were just monitoring the baby I would have been able to move freely, but the blood pressure monitor for me only had a few feet of slack. Luckily my sisters had arrived, and my mom and Norma soon after. My oldest sister Leise got to work decorating the room with tapestries and christmas lights. Norma put my birth playlist on, and she and my sister Josie danced next to the monitor with me, laughing at the appropriateness of the lyrics to "Push It". Every few minutes a contraction would hit me and I would grab my sister around the shoulders while Norma pushed on my back and helped me rotate my hips. My local doula Lisa had another woman in labor in the room next door, so it worked out perfectly that I already had so much support. She came in and out throughout my labor, and also called in her partner Sarah Boccolucci, who took the beautiful pictures and video that inspired this post. What this meant was that I had three doulas helping out during my labor in addition to my two sisters and my Nurse Midwife mom. And of course, my husband Max, who was my rock throughout. I felt so supported and loved, which turned out to be just what I needed. We waited for hours for the obstetrician on call to show up to say if I could come off the monitor, but she never came. In the meantime the nurse seemed to be increasingly distressed by my refusal to let her put a hep lock iv in. Later I would read my report and laugh at the description of me refusing the iv against medical advice because I have "big veins". I guess I really did say that. And I have no regrets. The last thing I wanted was to have a needle poking into my arm while in labor. After awhile the nurse said she could monitor my blood pressure intermittently so that I could have more slack. I took advantage to take a little walk in the hall and a lovely bath, with low lights and lavender bath salts. At last Dr. Shimoda arrived with the day shift and released me from the monitor. I was so glad she was on call that day. She had been the doctor we had interviewed when trying to decide whether to go with the ob group in Boulder. We had explained our desire for a natural birth, and asked questions about every possible scenario. Her straight forward answers and sarcastic wit had won me over. I knew she would stay out of my way unless I needed her, and I trusted that if she recommended an intervention it would be because it was necessary. Unfortunately the bath had worked too well to relax me, and my contractions were growing further apart, though still very intense. I reminded myself not to worry about it, but to be grateful for the break. I took the opportunity to eat some protein and rest, which my body craved. After awhile Max suggested we take a walk to get some fresh air. I couldn't leave the floor, but was allowed across the hall where there was an outdoor balcony. My acupuncturist, Monica Edlauer, found us there. We had made an appointment for her to come to the hospital that morning when we thought I was coming in for an induction. It turned out to be perfect timing. Each needle she put in seemed to bring my contractions closer together. By the time she was done I was in very active labor. Every contraction I felt that I needed to hold on to something above me and squat down. I had been using Max's shoulders for this, but I could tell he was getting tired. Lisa was there and suggested I try holding on to the top of the bed in a kneeling position. It turned out this is just what I needed. I felt the baby drop down, and a few contractions later my water burst with an amazing intensity. The nurse called Dr. Shimoda in to check how dilated my cervix was. "10 centimeters!" she said to my relief, "You can start pushing." This was the part that I had known was coming. It was the most painful part, pushing the baby out. "Don't fight it!" my mom said, "push into the pain." I had heard the rumor about ecstatic birth. These are women who experience pushing their babies out as one giant orgasm, and scream out of pleasure rather than pain. I decided to imagine that the pain I was experiencing was pleasure. I had used this technique to psych myself up for going to the hospital. By telling myself I was going to a wonderful hotel where all of my needs would be taken care of I was able to overcome my anxiety about having a hospital birth. So I told myself that I was about to have a giant orgasm. Lisa said "Breathe out fear, breathe in love", and I repeated this to myself as I imagined the pleasure I would feel as I pushed the baby out of my body, and the enormous relief once it was out. I screamed an enormous scream as I pushed as hard as I could through the next contraction. "Try to bring your voice down lower, push the baby towards your bottom." Lisa said. I focused on my breath, and the orgasm and the relief as I bore down during the next contraction. "I can see the baby's hair!" Max said, lifting my spirits as I knew that meant I was close to done. There was a nice pause before my next contraction, and I let myself relax against the bed until the next contraction began. The next contraction I thought "Open, love, orgasm, pleasure" as I pushed the baby's body out slowly, the pain increasing until finally he slipped out and there was a collective cry of amazement simultaneous with that great, wonderful relief. It was over, I made it through, I was on the other side now. 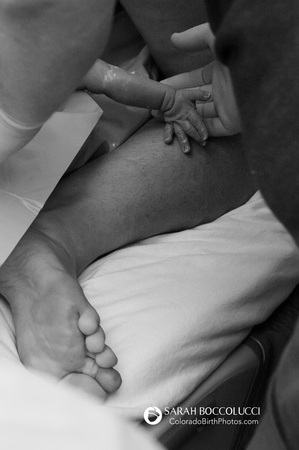 Everyone exclaimed with joy at the sound of the baby's first cry. "It's a boy!" Max told me, and slipped the baby through my legs so I could see him for the first time. "Be careful, his umbilical cord is short, he'll have to stay down here on your belly." my mom told me as she helped me turn over and lie down.  Dr. Shimoda congratulated me as she waited patiently for the cord to stop pulsing. I examined my baby as best I could, noting his perfectly formed fingers and toes, his cute little nose, and tiny ears. 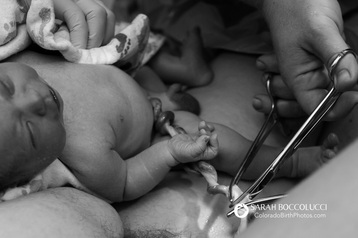 Max had been designated to cut the cord, and when it came time Dr. Shimoda talked him through it. The special care nurse we had met the week before was there. "We're just going to take him for a moment and give him some oxygen." she told me gently. Max followed her over to the warmer while Dr. Shimoda focused on me. "Are you feeling any cramping?" she asked as she tugged on the umbilical cord. I wasn't. "Can we give a small shot of Pitocin?" she asked, and explained that she was worried about hemorrhaging. Dr. Shimoda and I had a deal that if for some reason the baby had to be transferred down to Denver, she would release me as long as I had a normal vaginal delivery and was in good health. I had managed the first part, and didn't want to mess up our agreement by hemorrhaging. The nurse came and gave me a shot, and soon I pushed out the placenta. It was just a little sting, nothing compared to pushing out the baby, but it was still a relief when it was over. The special care nurse brought the baby over and handed him back to me to hold. "He needs a little bit of help, so I'm just going to keep this oxygen here." she told me as she held a plastic contraption near his mouth. I offered him my nipple and was ecstatic when he took it and began to suck. I had read that babies with Down syndrome have a hard time nursing. Not only that, but babies with congenital heart defects also have a hard time nursing. Since this baby had a double whammy, I had worried that he wouldn't be able to breastfeed. I had also worried that the joy of birth would be dampened by seeing the signs of Down syndrome in the baby's face. Max had been prepared that he might only see Down syndrome and not the baby, and had given himself a few months to learn to love the baby despite his diagnosis. This turned out not to be a concern. We were both immediately smitten with our baby, and neither of us saw Down syndrome at all. I even wondered at the time if there was a possibility the diagnosis had been wrong. Later it would be confirmed, and looking back at the pictures I can now see the signs of Down syndrome in Benny's newborn features. But it doesn't matter anymore. Now that we can hold him and see how wonderful he is, the diagnosis doesn't hold such huge anxiety for us. It's just a little part of who he is, like his red hair and his sparkling blue eyes. Those first few moments after the birth are what made all the pain of natural childbirth worth it. Holding my son skin to skin and looking into his eyes with the heightened love and joy of all that we had overcome and been through together is one of the most amazing and memorable moments of my life. I would never want to have numbed that. Without drugs in his system his natural instinct to breastfeed kicked in, giving us the advantage that we needed when over the next few hours it was determined that he needed extra help breathing and was put on a respirator and transferred down to a NICU in Denver. Thankfully, Dr. Shimoda kept her promise and released me from her care so that I could accompany him down to Denver. We weren't allowed to feed him for over 12 hours. Luckily, when I was finally able to put him to the breast, he remembered what he had learned in those first few moments, and was able to breastfeed successfully. After only four days we were able to bring him home from the NICU. We hadn't found out the gender of the baby ahead of time, and hadn't settled on a name either. So it was a week after he was born that we finally settled on his name. Benjamin, for three important people in Max's life: his close friend who had been charismatic and kind before he passed away too young; his grandfather Benny who had loved his family and his career as a violinist in the New York orchestra; and his Great-Uncle Benjamin, who broke boundaries and cultivated tolerance as the conductor of the first racially-integrated orchestra in the United States. That we would wish our child to be charismatic and kind, to love his family and his career and to break boundaries and cultivate tolerance seemed very fitting. And that is the story of how our baby Benny came into the world. |
Archives
April 2022
AuthorSince becoming a mom to a little boy with Trisomy 21 I have written a lot about Down syndrome and disabilities. I am a storyteller, wife and mom to a teen and a toddler. Life is busy! Categories
All
|














 RSS Feed
RSS Feed